 Tiny and deadly Tiny and deadly The worst outbreak in 30 years of yellow fever has hit the African country of Angola. Health care providers are attempting to head off the spread of this mosquito borne disease with a vaccination programme. They have vaccinated millions of Angolans but have many more to go and are rapidly depleting the stocks of vaccine. Prevention is the key to calming the latest epidemic. There is no cure once the virus takes hold of a person. Most people have flu like symptoms but about 15% go on to experience the severe form of the disease. Of those so stricken, half will die. As the disease progresses, it becomes a haemorrhagic fever and people bleed out. The flare up of the disease started in Luanda in mid-February and quickly escalated to 1600 confirmed cases. Two hundred twenty-five have died. Now the disease is moving into the DR Congo. There are a reported 21 fatalities to date with 151 confirmed cases. Some of those cases have been traced to the outbreak in Angola. The countries share a border. Currently, yellow fever is endemic in 44 countries. Africa and Latin America are the most strongly hit. WHO estimates that 60 000 people die from the disease each year. Those people who are planning travel to areas affected by this haemorrhagic disease are strongly urged to obtain a vaccination against the virus. Yellow fever is only one of a large number of haemorrhagic fevers that are largely confined to tropical areas. Mosquitoes are one of the insects that spread the viruses, but other biting insects are known to spread these diseases as well. More than 100 diseases are spread by arthropods. While most of these diseases are believed to have originated in tropical areas, they don’t always stay there. A combination of warming climate and quick travel can spread blood infections to new areas. An example of a recent introduction to N. America is the West Nile Virus. About 15 years ago a few cases were detected on the eastern US. Both people and horses were infected. Some infections spread by mosquito bites were mild but others led to complications and deaths. The disease now is established in most of the continent. Sources: CBC News WHO Microbiology and Immunology on-line
0 Comments
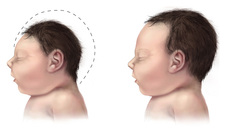 Comparison of microcephaly vs normal skulls Comparison of microcephaly vs normal skulls The Zika Virus is in the world’s headlines. It burst onto the world consciousness recently when thousands of babies in Brazil were born with abnormally small heads. Many of the newborns are healthy, but will require lifetime support. Not all micro encephalic babies survive. When an investigation of one deceased child was performed, the virus was found in its brain. Previously the Zika Virus was thought to be a relatively harmless invader that caused a mild reaction. Many people that had been infected were not aware of the virus in their blood stream. There’s more bad news about this emerging health problem. Zika is present in other South American countries as well. The health minister in Columbia is sounding the alarm about Guillain-Barre Syndrome(GBS). The virus is implicated in triggering the auto immune reaction that can cause paralysis, and in some cases, death. Normally few people present with GBS. Columbia is reporting hundreds of cases linked to Zika. “In the past week we have seen a substantial increase in the number of people reported with Guillain-Barré,” said health minister Alejandro Gaviria, referring to a rare syndrome that causes a person’s own immune system to damage nerve cells, leading to muscle weakness and sometimes, paralysis.” The Guardian WHO has declared the emerging Zika viral disease a “Public Health Emergency of International Concern”. The disease caused by the virus is known to spread by mosquitoes, but there is some anecdotal evidence that it can be passed human to human via body fluids. In Canada, the organization responsible for the blood banks has announced new regulations regarding donations from people suspected of exposure. Originally identified in Africa in 1947, the virus has now spread throughout Africa, the Middle East, India, SE Asia and Pacific Islands as well as S. America and Central America. At this time, countries that have cold winters seem to be immune to the mosquito that spreads the virus. Sources: National Institute of Neurological Disorders and Stroke The Guardian This last summer Erik Heil, Germany, participated in an Olympic test event in Guanabara Bay and contracted a flesh eating disease. He spent some painful time in a German hospital having the dead flesh scraped off his hips and legs.
Other athletes participating in the summer exercise came down with various ailments at a rate double that normally encountered. No count was kept of those who fell ill within two weeks of returning to their home countries. An expert in viral infections from Texas Health Center, Houston, Kristina Mena has stated that as little as three teaspoons of the Bay’s water ingested gives the athletes a 99% chance of being infected with a virus. The famous and scenic Copacabana Beach is dangerously polluted. Some of the water sports that will be held in the microbe laden waters:
“We’re talking about an extreme environment, where the pollution is so high that exposure is imminent and the chance of infection very likely.” The Guardian If any of the more than 10 000 athletes expected in the Brazilian city this August should fall ill with gastrointestinal or worse problems, they probably won’t find much comfort in their accommodations. As a cost saving measure it has been decided to not air condition the bedrooms of the athletes. Temperatures in August hover in the 35 degree Celsius range(95 Fahrenheit). In fact, electricity may be in short supply as a firm contract with the private electrical company has not been signed. The venue may have to depend on generator power. Sources: The guardian Lonely Planet Rio de Janeiro City Guide CBC  Tiger mosquito(Aedes albopictus) spreads disease Tiger mosquito(Aedes albopictus) spreads disease A little known emerging viral infection has gained a foothold in Florida. Chikungunya fever has spread from Africa to southern Asia and on to the Caribbean. It had been found sporadically in the USA in people who returned from areas where the disease was found. Recently a person developed Chikungunya without leaving Florida. The mosquito borne disease had a major outbreak in an island off Madagascar in 2005/2006. Approximately 300 thousand people contracted the painful disease. Mexico has recorded 7000 cases up to September 2015. The disease can sometimes be mistaken for Dengue Fever(breakbone fever) because severe joint pain is common for both. Encephalitis is sometimes part of the infection. Generally the very young and very old are most vulnerable to permanent neurological damage. The death rate hovers around 17%. There is no vaccination or cure. Pain killers can be used to help with the joint pain. Its name in the Makonde language, spoken in Tanzania and Mozambique in Africa, means "it bends up," because patients are often contorted with pain. They can spend weeks in bed, racked with pain. NBC News The Aedes mosquito is the vector for this disease. It survives best in warm climates. It flies and feeds in daytime or night. It is active inside and outside. Because prevention is so important, WHO advises that people wear clothing that covers skin and the wearing of repellents like DEET. It advises travellers to these tropic areas to only sleep where intact screens are in place or to stay where air conditioning means that windows are shut tight.
As the planet warms, diseases of the tropics are expected to more easily spread as the insect carriers make their way to new territories. Aedes albopictus(tiger mosquito) is already adapted to living in climates cooler than the tropics. This busy arthropod is a vector for yellow fever, dengue and worm parasites in addition to chikungunya. It was introduced to N. America from Asia in old tires that contained water. Sources: Science Daily CDC NBC WHO  DNA model DNA model Scientists working at the US National Institute of Health have made some intriguing discoveries about ALS aka Lou Gehrig’s Disease and officially as amyotrophic lateral sclerosis. It is a neurodegenerative disease which has no treatment and no cure. All people who develop it will have a shortened life span. They have found that in people with ALS have viral particles that have become activated. These viral particles have been carried along in the people’s DNA and become activated. Viral particles in human DNA are normal but usually not active. Often they simply sit there doing nothing and are referred to as “junk DNA”. Dr. Avindra Nath observed that sometimes people with HIV exhibited symptoms akin to ALS but these symptoms could be reversed with the use of antiviral drugs. It inspired him to study the possibility that a class of viruses known as retroviruses may have a role in causing the neuron destroying disease. They devised a study using a mouse model. The mice were genetically engineered to activate the retrovirus carried in their genetic code. They exhibited signs of death of motor neurons, the same neurons that die in humans with ALS. Then they treated some of the mice with an antiretroviral drug. The mice improved. It is very early days yet, but Dr. Nath is optimistic and has planned Stage 1 testing. We may have discovered a precision medicine solution for treating a neurodegenerative disorder," said Dr. Nath. Science Daily What triggers the start of this deadly disease is still unknown. There are two kinds of ALS – Sporadic and Familial. Familial presents a greater risk of developing the disease through inheritance. Sporadic trigger is unknown, but the ALS Association mentions that military veterans are twice as likely as the rest of the population to develop this neurodegenerative disease. Viruses are a strange group of infective particles. They are unable to reproduce on their own, but require the hijacking of a host’s DNA to reproduce. They stitch themselves into the genome of a host cell and subdue its defenses in order to produce more viral particles. Often the infected cell dies. Sometimes they stitch themselves into a host’s DNA and ride along for generations before causing a disease. Sources: ALS Association Science Daily National Institute of Neurological Disorders and Stroke |
Barbara McPherson
Blogger, gardener, farmer. Working toward food security and a 30 foot
diet. Addicted to reading. Love this planet, especially my little corner
on Vancouver Island, Canada Archives
October 2016
Categories
All
|


